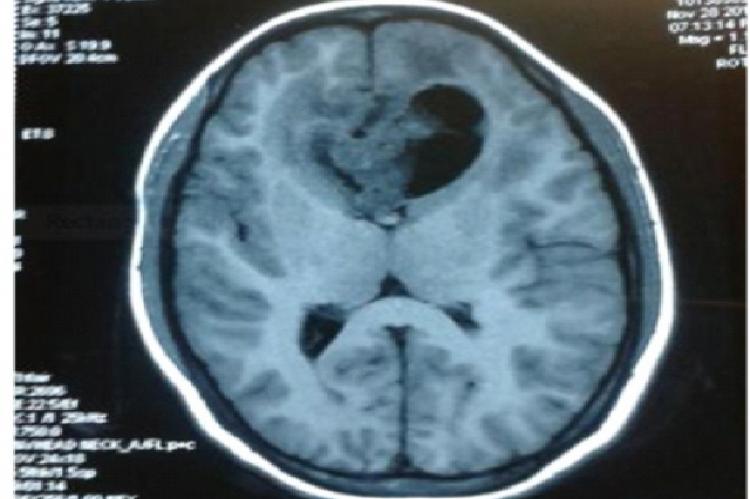
Glioblastoma (GBM) is the most common and most malignant among the glial tumours. Giant cell glioblastoma (GCG) is one of rare subgroup which constitutes around 5% of all GBMs. Histologically it is characterized by the presence of abundant bizarre, multinucleated giant cells along with abundant reticulin stroma and high frequency of p53 mutations. GCG more commonly involve the temporal and frontal lobe of brain. It portends a better prognosis than the usual GBM which were depicted in few case reports and studies. Treatment approaches in cases of GCG includes surgery followed by radiotherapy and chemotherapy.The aim of surgical intervention is to achieve maximal tumour excision with minimal morbidity leading to better quality of life.Atotal or subtotal resection can be achieved in greater percentage of patients (pts.) when advanced magnetic resonance imaging (MRI) techniques and intraoperative MRI techniques are used simultaneously. A newer concept about two types of GBM has been recently developed combining clinical, morphological and genetic data i.e. “primary” and “secondary” glioblastoma. Here we are sharing a case report of 27 year old lady who presented in our outpatient department (OPD) as a post-operative (post-op) case of GBM of corpus callosum for adjuvant radiotherapy. We evaluated the patient. and started radiotherapy with proper medical decompression and symptomatic management on OPD basis. After receiving 5th fraction of radiotherapy, patient.. condition deteriorated and in-spite of all resuscitative measures patient. expired on 3rd day of management in the Oncology ward.
View:
- PDF (684.98 KB)